
Rest has become a performance metric. Where previous generations simply went to bed and hoped for the best, a growing number of people in 2026 approach their nightly recovery with the same data-driven intensity they bring to training loads, nutritional tracking, and productivity optimisation. The market has responded accordingly. Sleep technology — encompassing wearables, smart mattresses, dedicated tracking devices, environmental control systems, and a sprawling ecosystem of apps — is now a multi-billion pound global industry, and it is expanding rapidly.
The question worth asking honestly, beneath the marketing language and the impressive dashboard visualisations, is whether any of it actually works. Whether the data these devices collect is accurate. Whether acting on that data produces measurable improvements in nightly rest quality. And whether the act of tracking your nights so obsessively might, in some cases, be making things worse rather than better.
The answers are more nuanced than either enthusiastic adopters or sceptical critics tend to acknowledge — and understanding them requires looking at the technology, the science, and the psychology simultaneously.
The first thing to understand about consumer rest technology is what it is actually capable of measuring, as distinct from what it claims to measure. This distinction matters considerably, because the gap between the two is where most of the legitimate criticism of the category lives.
Clinical assessment — the gold standard — is conducted through polysomnography, a process involving electrodes attached to the scalp, face, and body that measure brain electrical activity, eye movements, muscle tone, heart rate, respiratory effort, and blood oxygen saturation simultaneously throughout a night's rest. This data allows trained clinicians to identify sleep stages with high precision, diagnose disorders including sleep apnoea, restless leg syndrome, and parasomnias, and make treatment recommendations grounded in direct physiological measurement.
Consumer devices measure none of this directly. What they actually measure is a combination of movement, heart rate, heart rate variability, skin temperature, blood oxygen saturation, and respiratory rate — all of which are correlates of sleep stages rather than direct measurements of them. The algorithms that translate accelerometer data and heart rate patterns into “deep sleep,” “light sleep,” and “REM” classifications are proprietary, vary between manufacturers, and produce results that independent research has found to be inconsistent when compared against polysomnographic reference data.
This is not a trivial limitation. Studies comparing consumer wearable staging against clinical polysomnography have consistently found that devices perform reasonably well at distinguishing rest from wakefulness but significantly less well at identifying specific stages — overestimating deep sleep in some studies, misclassifying REM in others. The confidence with which apps present breakdowns — “you spent 94 minutes in deep sleep last night” — is not always warranted by the underlying measurement quality.
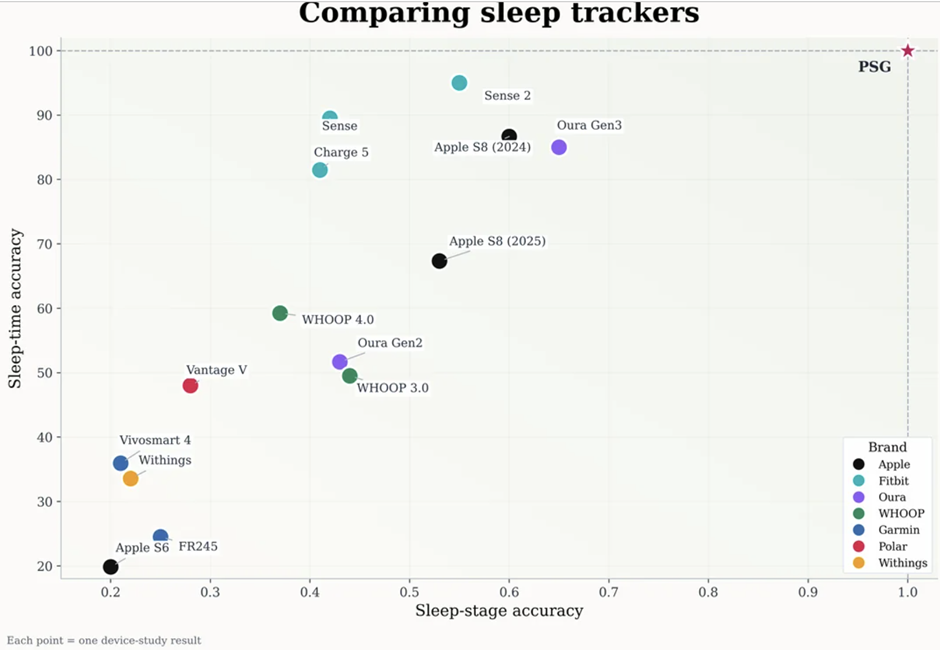
The most significant development in tracking hardware over the past three years has been the mainstream success of the smart ring form factor. Devices from Oura, Samsung, and a growing field of competitors have demonstrated that a ring worn on the finger can collect physiological data with quality comparable to — and in some metrics superior to — wrist-worn devices, while being more comfortable to wear at night and less intrusive in daily life.
The finger is, from a physiological measurement perspective, a genuinely good location for optical heart rate and blood oxygen sensors. The blood vessels are close to the surface, the signal is strong, and movement artefacts that compromise wrist-based readings during the night are reduced. Temperature sensing at the finger also produces more stable and consistent data than equivalent sensors on the wrist, which is particularly relevant for tracking the circadian temperature rhythms that correlate with rest quality and — in the Oura ring's most clinically validated feature — provide early warning signals for illness and physiological stress.
The Oura Generation 4, released in late 2024, and its 2026 competitors have pushed the form factor's capabilities further: continuous blood oxygen monitoring, improved movement classification, and algorithmic refinements trained on larger datasets than earlier generations. The devices have also expanded their health monitoring scope beyond sleep, which raises the question of whether “sleep tracker” remains an adequate description of what they actually are. In a broader sense, the seamless integration of these tools into everyday routines mirrors the ease of accessing modern digital platforms — much like using a Hiddenjack inloggen, where complex systems operate behind a simple, user-friendly interface.
Smart Mattresses: The Most Ambitious Hardware in the Category
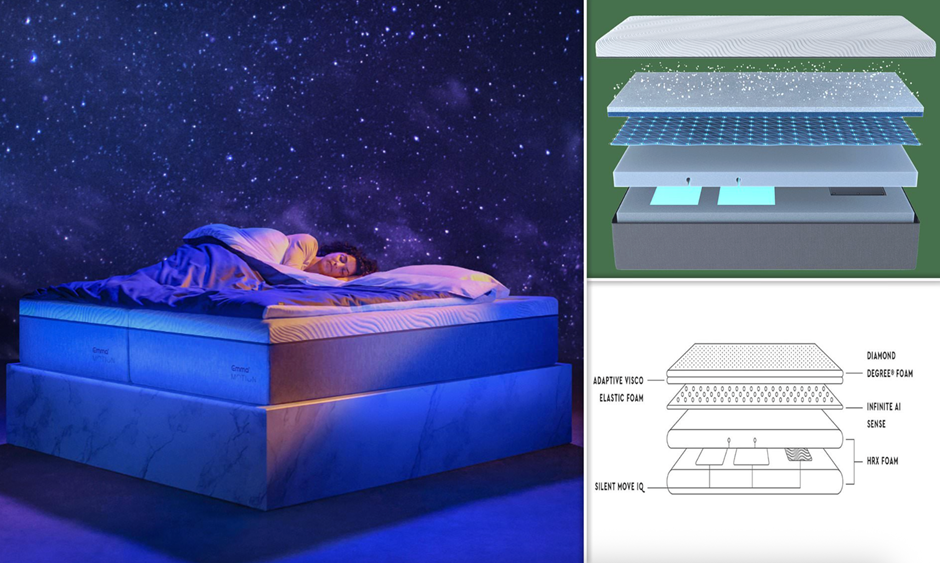
At the premium end of the market, smart mattresses from companies including Eight Sleep and Sleep Number represent the most comprehensive — and most expensive — approach to nocturnal optimisation. These products combine sensing capability with active environmental intervention, monitoring the sleeper's physiological signals while simultaneously adjusting mattress temperature, firmness, and elevation in response to what the system detects.
Eight Sleep's Pod series, which has continued to develop through successive generations, is the most technically sophisticated product in this category. The mattress cover contains a network of sensors monitoring movement, heart rate, and respiratory rate, feeding data to algorithms that adjust the water-based temperature regulation system throughout the night in response to detected stages and physiological signals. The claimed benefit is that maintaining optimal temperature during each phase — cooler during deep sleep, slightly warmer during REM — enhances the quality and duration of restorative rest.
The independent evidence for temperature-based nocturnal optimisation is genuine and reasonably well-established in the relevant science. Core body temperature naturally falls during the transition to sleep and reaches its lowest point during deep slow-wave sleep. Environments that support this cooling process are associated with better architecture across the night. The question is whether the active temperature adjustment these systems provide produces improvements beyond those achievable through simpler means — appropriate bedding, a well-ventilated room, thermostat management — and whether the price premium is justified by the marginal benefit.
User-reported outcomes for premium smart mattresses are generally positive, but self-reported data is subject to placebo effects that are particularly difficult to control in rest research. Independent controlled studies of these specific products remain limited relative to the strength of the marketing claims.
The Orthosomnia Problem: When Tracking Makes Things Worse
In 2017, researchers coined a term that has become increasingly relevant as tracking technology has proliferated: orthosomnia. Derived from the Greek for “correct” or “straight,” it describes the anxiety and disruption that can arise from excessive focus on achieving perfect tracker scores.
The phenomenon is straightforward in its mechanics. A person begins monitoring their nights with the intention of improving them. They receive data suggesting their deep sleep duration is below average, or their efficiency score falls short of the app's target range. They begin focusing on achieving better scores — going to bed earlier, lying very still to avoid movement being registered as wakefulness, avoiding activities they associate with lower scores. The monitoring itself becomes a source of pre-bed anxiety, which is precisely the psychological state most likely to disrupt the restorative architecture they are trying to improve.
Clinical case reports of orthosomnia describe patients who have developed genuine insomnia as a direct result of tracking, in some cases requiring therapeutic intervention to restore a healthy relationship with rest. The irony is considerable: technology marketed as a solution to poor nights can, in susceptible individuals, become a cause of them.
The implication is not that tracking is harmful for everyone — most users engage with the data in ways that remain psychologically healthy. It is that the technology is not appropriate for everyone, and that people with existing anxiety or perfectionistic tendencies should approach these devices with particular care.
What the Science Says About Effective Sleep Improvement
Given the limitations of sleep tracking technology and the genuine risk of orthosomnia in some users, it is worth being clear about what sleep science has actually established as effective for improving sleep quality — because the evidence base here is considerably stronger than for most of the technology category.
Sleep hygiene — the collection of behavioural and environmental practices that support good sleep — has robust evidence behind it. Consistent sleep and wake times that anchor the circadian rhythm. A sleeping environment that is dark, quiet, and cool. Avoiding bright light exposure in the hour before bed, which suppresses melatonin production and delays sleep onset. Limiting caffeine consumption after early afternoon. Regular physical activity, timed appropriately to avoid raising core body temperature immediately before sleep.
Cognitive behavioural therapy for insomnia — CBT-I — is the most evidence-supported treatment for chronic insomnia available, with outcomes that outperform sleep medication in long-term follow-up and no adverse effects. Digital CBT-I programmes, delivered through apps and online platforms, have made this intervention accessible at scale in ways that were previously impractical.
The most valuable thing a sleep tracking device can potentially do is motivate behaviour change in the direction of these evidence-supported practices — reinforcing consistent sleep timing, identifying how caffeine or alcohol consumption affects measured sleep quality, and providing feedback that connects behavioural choices to physiological outcomes. When used as a tool for that kind of behavioural reinforcement rather than as a target to optimise obsessively, the technology has genuine utility.
The Honest Verdict
Sleep technology in 2026 sits in a complicated position: more capable than its critics acknowledge, less reliable than its marketing suggests, and genuinely useful for some people while potentially counterproductive for others. The hardware has improved substantially. The measurement accuracy for key metrics — heart rate, temperature, blood oxygen — is now strong. Sleep stage classification remains an estimate rather than a measurement. The difference matters.
For people who engage with the data lightly — using trends over weeks rather than obsessing over nightly scores, and treating the technology as a nudge toward better habits rather than a target to maximise — sleep technology can be a worthwhile investment. For people prone to health anxiety or perfectionism, the psychological risks deserve serious consideration before purchase.
The best sleep technology, ultimately, is the kind that disappears into the background and quietly supports better habits without becoming a source of pressure in its own right. The devices that achieve that balance are worth the money. The ones that turn your bedroom into a biometric performance review are not.
Have you used sleep tracking technology? Did it help — or did it make things more complicated? Share your experience in the comments, and pass this article on to anyone considering investing in sleep tech.





